The Impact of Sleep Apnea on Mental Health: What You Need to Know

Introduction
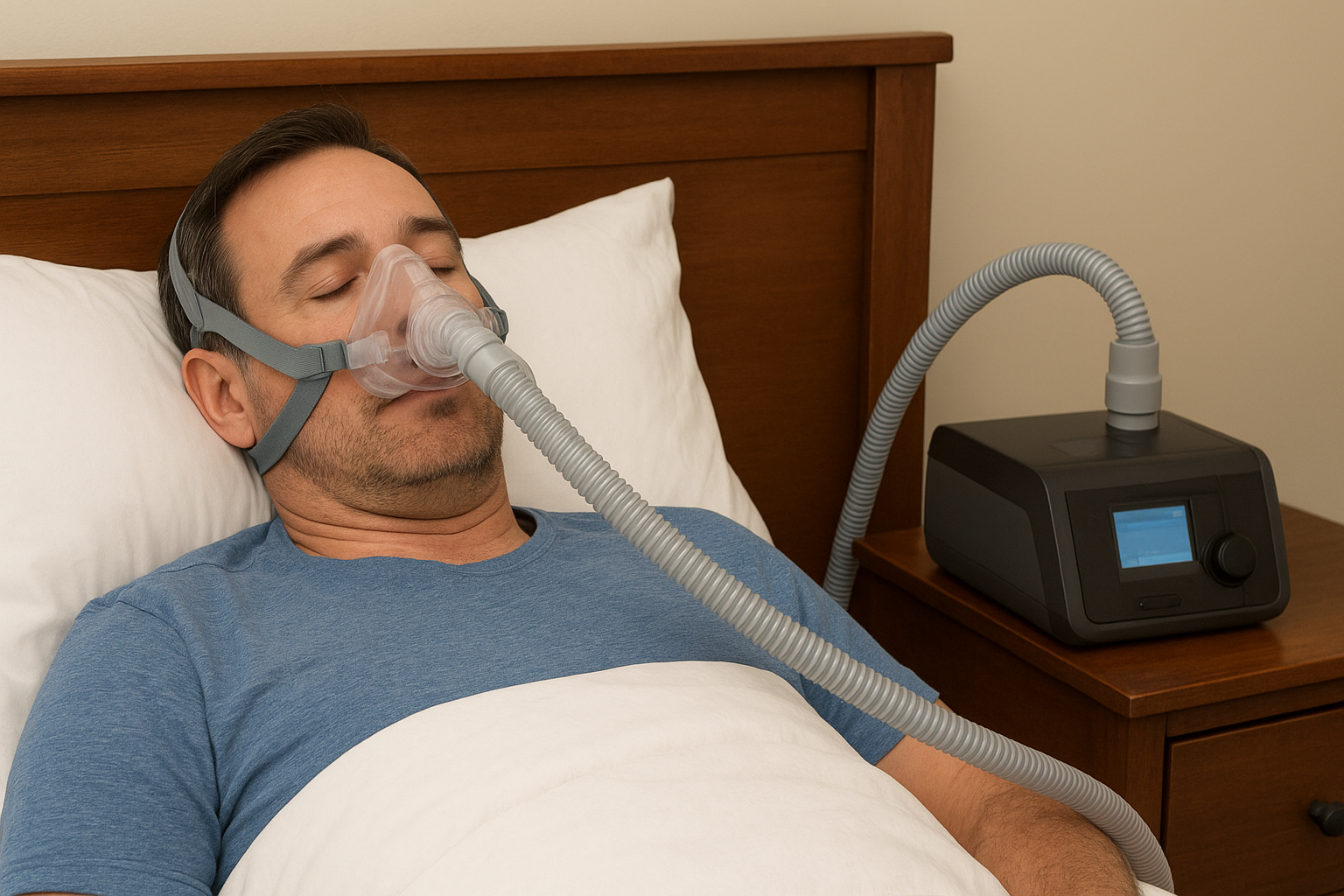
Obstructive Sleep Apnea (OSA) is a widespread sleep disorder affecting millions worldwide, including a significant number in the United States. Characterized by repeated interruptions of breathing during sleep, OSA often leads to fragmented, non-restorative sleep, yet its impact goes far beyond physical fatigue. In particular, OSA can significantly affect mental health—leading to or exacerbating conditions like depression, anxiety, cognitive dysfunction, and even increased risk for neurological diseases. Fortunately, the CPAP machine, the gold-standard therapy for OSA, offers meaningful relief not only for physical symptoms but also for mental well-being. This article explores the relationship between sleep apnea and mental health, explains why CPAP therapy is so vital, and offers actionable advice for both clinicians and patients.
1. Understanding the Link: Sleep Apnea and Mental Health
1.1 Psychological Toll of OSA
Sleep apnea is strongly associated with mental health issues. Patients with OSA exhibit higher rates of depression (up to 46%) and anxiety (around 30%) compared to the general population (Sleep Healthy PA |). The mechanisms behind this include sleep fragmentation, oxygen deprivation, and elevated stress hormones, which collectively disrupt mood regulation and emotional stability (Sleep Healthy PA |, WIRED).
Intermittent hypoxia—the recurring drops in blood oxygen—can damage brain regions responsible for emotional control and cognitive function (WIRED, 维基百科). This damage can initiate or worsen mood disorders and cognitive impairments.
1.2 Cognitive and Emotional Consequences
The link between OSA and cognitive decline is well-documented. Sleep fragmentation and hypoxia contribute to memory impairment, reduced attention span, and impaired executive function. A longitudinal study found that untreated, sleep-related breathing disorders can lead to earlier onset of mild cognitive impairment—potentially accelerating the development of Alzheimer’s disease—by up to 10 years (WIRED, TIME).
Beyond cognition, the disruption of REM sleep—critical for emotional processing—can intensify emotional dysregulation and depressogenic symptoms (WIRED).
2. Why the CPAP Machine Matters
2.1 CPAP: The Gold Standard for OSA Treatment
Continuous Positive Airway Pressure (CPAP) therapy remains the primary and most effective treatment for moderate to severe OSA. It maintains an open airway during sleep by delivering steady airflow through a mask (Yale Medicine, 维基百科). Modern CPAP devices feature improved mask designs, automatic pressure adjustment, and remote monitoring capabilities (Yale Medicine).
2.2 Benefits for Mental Health and Cognition
Use of CPAP has been shown to reduce depression and anxiety symptoms, especially when used effectively (over 4 hours per night) (SAGE Journals, Dove Medical Press). A meta-analysis confirms significant psychological improvements with consistent CPAP use (SAGE Journals). In moderate to severe OSA cases, CPAP improved sleepiness, quality of life, and cognitive function (Dove Medical Press).
Longitudinal studies show that CPAP use for 12 months decreases depressive symptoms and enhances emotional regulation (科学直通车). Moreover, CPAP significantly boosts subjective mood, quality of life, and cognitive functions—such as memory, attention, executive function—over three to six months (MDPI).
2.3 Physical Health Benefits That Support Mental Well-being
Untreated OSA causes spikes in blood pressure, heart rate, blood sugar, and stress hormones—physiological stressors that elevate mental health burden (霍普金斯医学). Regular CPAP use stabilizes these parameters and consequently improves wakefulness and quality of life (霍普金斯医学).
3. Challenges in CPAP Therapy and Enhancing Adherence
3.1 Common Difficulties
Many users struggle with CPAP due to issues like mask discomfort, leaks, nasal congestion, dry mouth, or claustrophobia (Mayo Clinic, 维基百科). These can lead to poor adherence or abandonment of therapy, which undermines both physical and mental health benefits.
3.2 Strategies for Better Adherence
Patient education, support, and care coordination are key. A clinically integrated care model reported 90% current CPAP usage, compared to 54% in traditional models. Satisfaction across testing, adoption, ongoing support, and quality of life was significantly higher in the integrated model (Frontiers).
Behavioral interventions such as cognitive behavioral therapy (CBT), motivational enhancement, and exposure therapy for claustrophobia have proven effective in improving CPAP adherence—sometimes by as much as 148% (维基百科).
4. Why Addressing CPAP Adherence Matters for Mental Health
By leveraging CPAP effectively—especially with supportive clinical programs—patients are more likely to experience relief not just from physical symptoms but also improvements in mood, cognition, and emotional regulation. This holistic benefit extends to better performance at work, improved social functioning, and enhanced overall quality of life (Frontiers, MDPI, GQ).
The narrative of one patient illustrates the stakes: after years of fatigue, irritability, and memory issues, receiving a CPAP machine dramatically improved his energy, mood, and mental clarity (GQ).
5. Practical Takeaways and Recommendations
For Patients:
- Use your CPAP machine consistently (ideally >4 hours nightly) to reap mental health benefits.
- Seek help if you experience discomfort—adjust mask fittings or try alternative models.
- Engage in care programs or behavioral therapies that support CPAP adoption and adherence.
For Clinicians:
- Educate patients about the mental health impacts of OSA and the broader benefits of CPAP.
- Encourage integrated care models and behavioral support to boost cases where CPAP is challenging.
- Monitor mood, cognitive symptoms, and quality of life routinely in OSA management.
Conclusion
Sleep apnea exerts a profound impact on mental health—affecting mood, cognition, emotional regulation, and even accelerating neurological decline. Yet, the CPAP machine, when used effectively and supported properly, offers a powerful intervention. By treating OSA, patients can not only sleep better but also regain mental clarity, emotional balance, and improved quality of life. With enhanced awareness, adherence support, and integrated care, we can ensure that individuals struggling with OSA receive the full spectrum of benefits they deserve.
Key Takeaways:
- OSA significantly raises the risk of depression, anxiety, and cognitive decline.
- CPAP therapy is clinically proven to improve sleep, mood, cognition, and physiological health.
- Common barriers to CPAP can be overcome through support, education, and behavioral strategies.
- Improved CPAP adherence translates into better mental health outcomes and overall well-being.